People Aging with HIV are Facing Significant Barriers in the Healthcare System Undermining and Disrupting their HIV Clinical Progress and Broader Health Outcomes

HealthHIV’s Fifth Annual State of Aging with HIV™ National Survey Identifies Issues Across Five Connected Domains: HIV and Geriatric Care, Comorbidities, Mental and Behavioral Health, Access and Payment, and Workforce
FOR IMMEDIATE RELEASE
May 15, 2026
WASHINGTON, D.C. — People aging with HIV face significant barriers and critical disruptions in care and treatment that undermine their clinical progress and social support, according to a just released report on the findings from HealthHIV’s Fifth Annual State of Aging with HIV National Survey. The survey revealed the daunting reality of aging with HIV, including managing multimorbidity and frailty risk, mental health challenges, and the structural barriers they face regularly.
Adults aged 50 and older already represent more than half of all people living with HIV in the U.S., and are projected to account for 70% by 2030. They face significant barriers and critical disruptions at every step in care and treatment that undermine their clinical progress and social support. The survey report describes the findings and implications of these and other issues, and how the next phase of HIV care has to pivot toward the needs of aging with HIV across five connected domains—HIV and Geriatric Care, Comorbidities, Behavioral Health, Access and Payment, and Workforce.
Over the past five surveys, consumers reported high rates of viral suppression. “These results reflect often hard-won clinical gains that can quickly erode when continuity of care is disrupted,” says Dr. Circe Gray Le Compte, Senior Director of Research and Evaluation at HealthHIV. “During COVID-19, suppression rates among people aging with HIV dipped sharply as consumers were cut off from care. Low-income, women, and transgender/gender nonconforming persons aging with HIV experienced even sharper declines.”
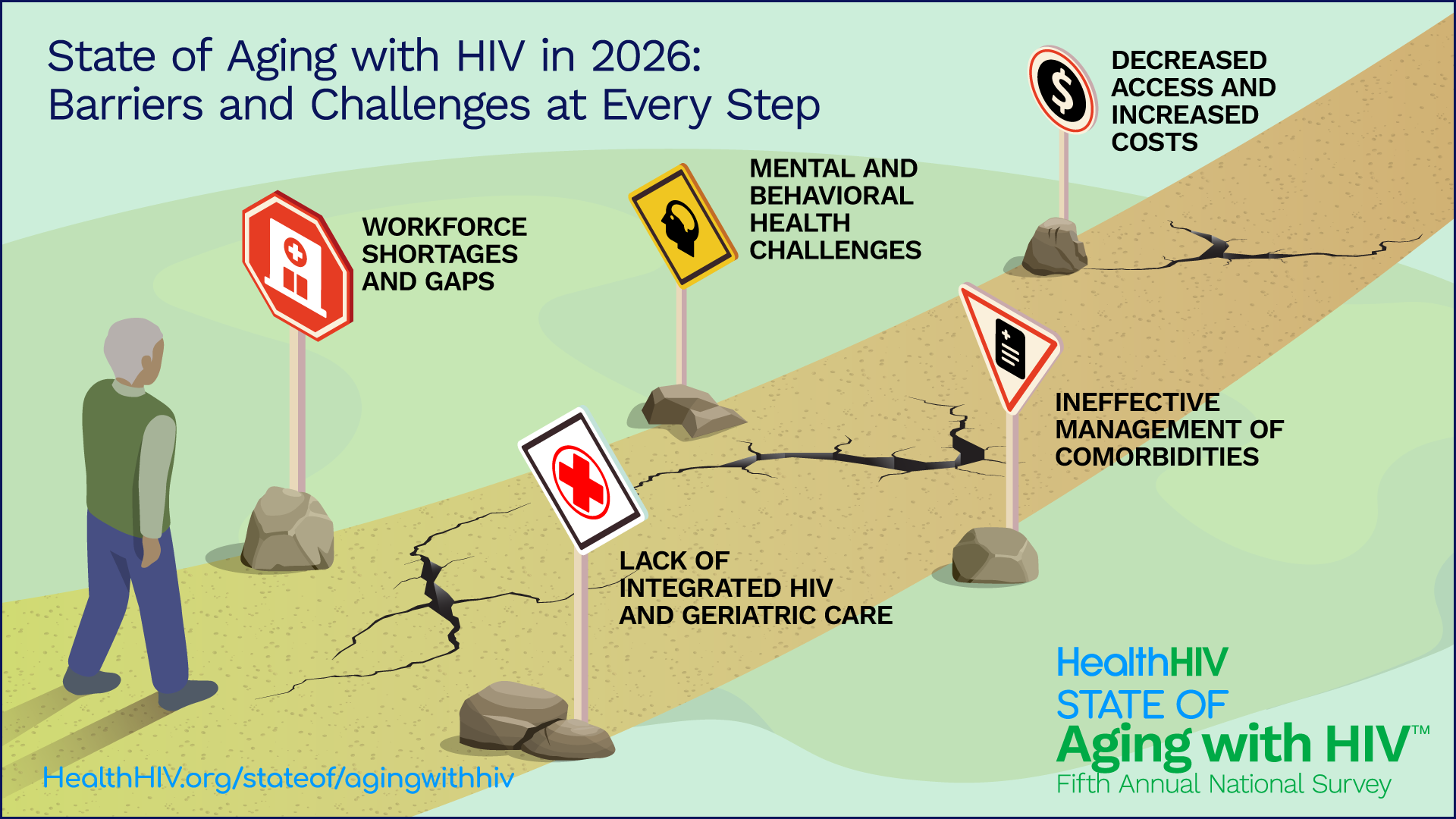
Survey Findings and Implications include:
- HIV and Geriatric Care
Finding: Viral suppression of 98% is the highest rate since HealthHIV started collecting data in 2020, yet aging with HIV is not being managed at the same level. This is especially true for low-income and sexual and gender minorities, whose connection to care declines more quickly under stress, as we saw during COVID-19.
Implication: Bolster infrastructure that supports this suppression rate to integrate frailty and geriatric screening into Ryan White HIV/AIDS Program (RWHAP)-funded clinical visits. - Comorbidities
Finding: Most consumers carry chronic non-HIV medication burden, and a high-needs unmanaged group is invisible to every system except HIV antiretroviral (ART) therapy. Respondents cited suboptimal management of comorbidities.
Implication: Fund clinical pharmacist consultations as a reimbursable RWHAP service category; reauthorize and align the Older Americans Act with earlier-onset aging-related needs so that supports are not limited by chronological aging. Better clinically address comorbidities including frailty risk, cardiovascular disease, and mental health burden. - Behavioral Health
Finding: Stress is widespread, while social connection is the strongest protective factor in the data; outwardly good quality of life can mask serious mental health burden.
Implication: Make mental and behavioral health screening a default in HIV primary care, and treat anti-discrimination training as a clinical intervention. - Access and Payment
Finding: Medication coverage is doing what it was designed to do, but the surrounding infrastructure, including payment and transportation, is fragile, with ART access no longer assumed to be stable.
Implication: Support treatment access by treating transportation as essential medical infrastructure, making Medicare telehealth permanent for HIV care, and stabilizing the AIDS Drug Assistance Program (ADAP) rebate base. - Workforce
Finding: Most providers recognize that aging with HIV is a clinical priority, but few organizations have the staffing, training, or workflows to act on that recognition. Workforce turnover is eroding the practical knowledge needed to deliver aging-informed care.
Implication: Nonprofits and government agencies need to provide more education and training for the workforce addressing HIV and geriatric care. Supporting the geriatric needs of people aging with HIV has outpaced operational capacity. Less than one-fifth of consumers completing the survey reported receiving frailty screening in the past year, while many described dealing with often unaddressed mental health concerns and limited social support.
“People aging with HIV are navigating far more than the virus itself, even as viral suppression and sustained care remain unevenly supported across fragmented systems,” states HealthHIV Director of Advocacy and Pozitively Aging Program Lead Scott Bertani. “This survey reflects growing strain across care and prevention access, financial stability, mental health and the ability of providers and systems to keep pace with increasingly complex health needs and lived social realities.”
When asked to describe aging with HIV in a single word, both consumers and providers most often chose “challenging,” “difficult,” and “complicated”—a pattern consistent with findings from the previous two surveys. One notable difference emerged around loneliness: providers identified it more frequently than consumers, suggesting that social isolation may be recognized by others before individuals acknowledge it themselves.
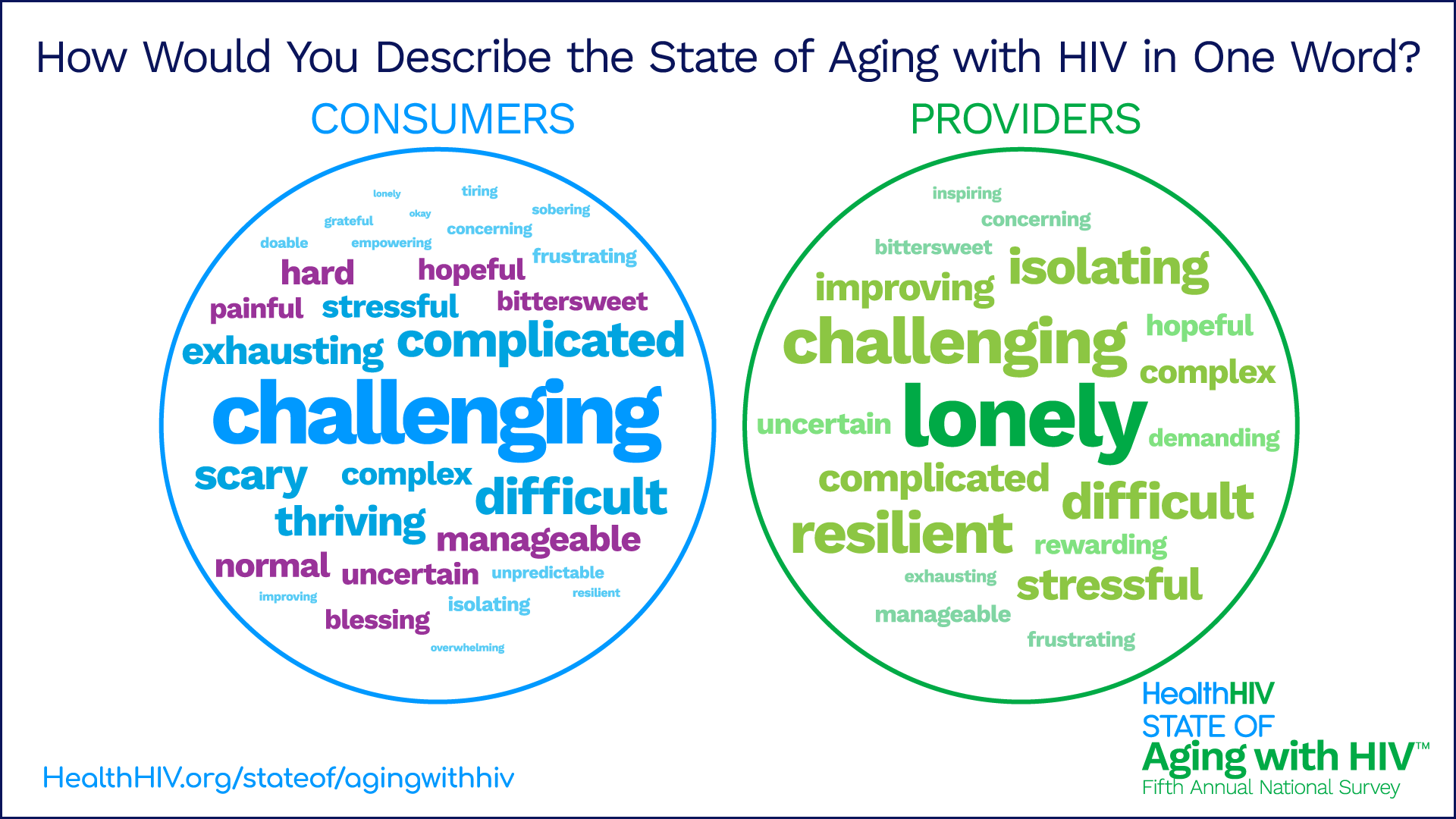
A report on Findings and Implications from HealthHIV’s Fifth Annual State of Aging with HIV National Survey is available to view and download on the HealthHIV website at HealthHIV.org/stateof/agingwithhiv.
About the HealthHIV Fifth Annual State of Aging with HIV™ National Survey
The survey, conducted as part of HealthHIV’s Pozitively Aging program, which is supported by Gilead Sciences through their HIV Age Positively initiative, examines crucial issues facing people aging with HIV and HIV-aging service providers. The 2026 cohort encompassed 706 respondents representing 37 U.S. states and the District of Columbia: 365 consumers (people with HIV aged 50 and older and/or living with HIV for 15 or more years) and 341 behavioral and clinical providers who deliver services to people aging with HIV. Data were collected between February and March 2026 via REDCap nationwide. Our analysis of the data and presentation of the findings and associated implications point to where change is most needed and what kinds of support could make the biggest difference, both for people aging with HIV and for the workforce caring for them.
HealthHIV encourages the aging with HIV community to use the findings to guide the development and prioritization of education and training efforts and materials for the HIV care workforce and inform advocacy and research priorities. To access the survey report, please visit HealthHIV.org/stateof/agingwithhiv.
About the Pozitively Aging Program
HealthHIV’s Pozitively Aging program empowers Persons Aging with HIV, including Long-Term Survivors, Individuals >65, Lifetime Survivors (“Dandelions”), and those with unmet needs. The program addresses systemic inequities, enhances workforce capacity, and strengthens care coordination through training, education, advocacy and research.
The Pozitively Aging program offers resources and tools supporting aging with HIV. These include the Healthy Aging Hub, the Healthy Aging with HIV Series Certificate Program, the Annual State of Aging with HIV™ National Survey, and a range of advocacy activities. The Healthy Aging Hub serves as a practical hub for a wide range of materials including policy and advocacy, provider education and curricula, research and practice insights, and community-facing resources.
The Healthy Aging with HIV Series Certificate Program explores what it means to age with HIV, connecting science with lived experience and everyday practice. It is a tool for providers, case managers, peer navigators, and advocates to learn about the intersection of medical knowledge with workforce readiness, social determinants of health, and supportive care systems. Learn more at healthhiv.org/pozitivelyaging.
About HealthHIV’s “State Of” Surveys
HealthHIV Research and Evaluation conducts regular national surveys to better inform ongoing advocacy, education, research, and training activities. These “State Of” surveys provide unique insight into patient and provider issues in order to optimize primary and support services for diverse communities. The regular reports offer the ability to report multi-year trends illustrating changes, challenges, and opportunities to address the needs of providers and patients. HealthHIV, HealthHCV, and the National Coalition for LGBTQ Health conduct “State Of” surveys addressing HIV Care, HCV Care, LGBTQ Health, Harm Reduction, and Aging with HIV. Learn more at healthhiv.org/stateof.

